Sinus Headaches and Migraines: Symptoms, Causes, and Differences
Headaches are a common ailment that most of us have experienced at some point in our lives. They can range from mild discomfort to debilitating pain, affecting our daily activities and overall well-being. Two types of headaches that are often confused due to their overlapping symptoms are sinus headaches and migraines. In this comprehensive guide, we will delve into the anatomy of sinuses, explore the symptoms and causes of both conditions, highlight their key differences, and emphasize the importance of accurate diagnosis and appropriate treatment.
Understanding Sinus Headaches
1. Anatomy of the Sinuses
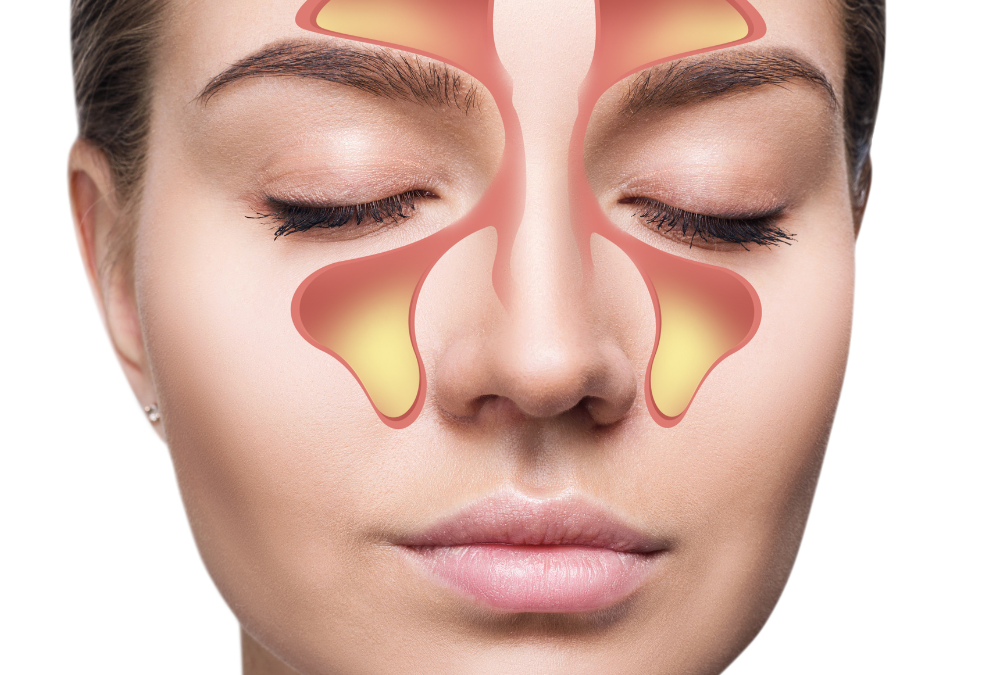
To understand sinus headaches, it’s crucial to first grasp the basics of the sinus system. The sinuses are a series of interconnected, air-filled cavities located within the bones of the skull and facial area. They serve several essential functions, including humidifying and filtering the air we breathe, enhancing vocal resonance, and reducing the weight of the skull.
There are four pairs of sinuses:
- Frontal sinuses (above the eyes)
- Ethmoid sinuses (between the eyes)
- Sphenoid sinuses (behind the eyes)
- Maxillary sinuses (within the cheekbones)
These sinuses are lined with a mucous membrane that produces mucus to keep the nasal passages moist and free of foreign particles.
2. Symptoms of Sinus Headaches
Sinus headaches typically manifest with the following symptoms:
Pain and pressure in the face: The most prominent symptom of a sinus headache is a dull, aching pain and pressure felt around the forehead, cheeks, and eyes. This discomfort is often exacerbated when bending forward or applying pressure to the face.
Nasal discharge: People with sinus headaches frequently experience nasal discharge. The mucus may be thick and discolored, which is a sign of inflammation or infection in the sinuses.
Fever and fatigue: When a sinus infection is the underlying cause, fever and fatigue may accompany the headache. These systemic symptoms are indicative of an ongoing infection.
Swelling around the eyes: Sinusitis, a common cause of sinus headaches, can lead to swelling and puffiness around the eyes. This is often referred to as periorbital edema.
3. Causes of Sinus Headaches
Sinus headaches are primarily caused by issues related to the sinuses themselves. Common causes include:
Sinusitis (acute and chronic): Inflammation of the sinus lining due to infection or allergies can lead to sinus headaches. Acute sinusitis is usually short-term and results from infections, while chronic sinusitis persists for more than 12 weeks and is often related to structural issues.
Allergies: Allergic reactions to airborne allergens, such as pollen, dust mites, or pet dander, can trigger sinusitis and subsequent sinus headaches in susceptible individuals.
Nasal polyps or structural abnormalities: Structural abnormalities in the nasal passages or the presence of nasal polyps can obstruct the normal flow of mucus and air, leading to sinus congestion and headaches.
Diving into Migraines
1. What is a Migraine?
Migraines are a neurological disorder characterized by recurrent, severe headaches that can be disabling. They are different from tension-type headaches and sinus headaches due to their distinct features and underlying causes. Migraines can vary in duration and intensity but typically present with specific symptoms.
2. Symptoms of Migraines
Common migraine symptoms include:
Throbbing or pulsing pain, usually on one side: Migraine headaches often involve intense, throbbing pain that is localized to one side of the head. However, they can also affect both sides or shift sides during an attack.
Sensitivity to light, noise, and sometimes smells: Migraine sufferers often become extremely sensitive to sensory stimuli, such as bright lights, loud noises, and certain odors. This heightened sensitivity can worsen the pain during an attack.
Nausea or vomiting: Many migraine sufferers experience gastrointestinal symptoms, including nausea and vomiting, during an attack.
Vision disturbances (auras): Some individuals with migraines experience visual disturbances known as auras before or during an attack. These can include flashing lights, blind spots, or zigzag lines in the field of vision.
3. Causes and Triggers of Migraines
Migraines can have various genetic and environmental factors contributing to their onset. Common triggers and causes include:
Genetic factors: Migraines tend to run in families, suggesting a genetic component to the condition.
Hormonal changes: Hormonal fluctuations, particularly in women, can trigger migraines. This includes menstruation, pregnancy, and menopause.
Food additives, caffeine, stress, etc.: Migraine attacks can be triggered or exacerbated by certain dietary factors, such as the consumption of specific foods and beverages (e.g., aged cheeses, caffeine, alcohol) and emotional stress.
Key Differences
1. Origin of Pain
Sinus: Pain in sinus headaches is derived from inflamed sinuses. The pain is typically localized around the face and head and is directly related to sinus issues.
Migraine: Migraines, on the other hand, are neurological in nature. The pain originates in the brain and is often accompanied by abnormal brain activity.
2. Associated Symptoms
Sinus: Sinus headaches are often accompanied by symptoms related to sinus inflammation, such as congestion, fever, and thick nasal discharge.
Migraine: Migraines come with a distinct set of symptoms, including aura, light sensitivity (photophobia), noise sensitivity (phonophobia), and nausea.
3. Duration
Sinus: Sinus headaches can persist as long as the underlying condition, such as sinusitis or allergies, continues. They tend to resolve once the underlying issue is treated.
Migraine: Migraines typically last between 4 to 72 hours, with a clear onset and resolution of symptoms during an attack.
4. Treatment Approaches
 Sinus: The treatment approach for sinus headaches focuses on targeting the underlying cause. This may involve antibiotics for bacterial infections, antihistamines and decongestants for allergies, or surgical intervention for structural abnormalities.
Sinus: The treatment approach for sinus headaches focuses on targeting the underlying cause. This may involve antibiotics for bacterial infections, antihistamines and decongestants for allergies, or surgical intervention for structural abnormalities.
Migraine: Migraine treatment includes pain relievers, such as NSAIDs or acetaminophen, as well as specific migraine medications known as triptans. Preventive medications are also prescribed for individuals with frequent or severe migraines.
Importance of Correct Diagnosis
Misdiagnosis of sinus headaches and migraines can lead to inadequate treatment and prolonged suffering for patients. Here are some of the key reasons why it’s crucial to differentiate between the two conditions:
Ineffective treatment: Treating a migraine as a sinus headache with antibiotics, for example, is not only ineffective but can also contribute to antibiotic resistance. Similarly, using migraine medications for sinus headaches may provide no relief.
Delay in appropriate treatment: Misdiagnosis can delay the initiation of proper treatment, allowing the underlying condition to worsen. For instance, untreated sinusitis can lead to complications such as chronic sinusitis or the spread of infection to nearby structures.
Impact on patient well-being: Both sinus headaches and migraines can significantly affect a person’s quality of life. Misdiagnosis may result in prolonged suffering and decreased productivity.
Diagnostic Procedures, Tests, and Treatments
Healthcare professionals rely on various methods to differentiate between sinus headaches and migraines:
Imaging tests: X-rays, CT scans, or MRI scans may be used to visualize the sinuses and rule out structural abnormalities, infections, or sinusitis.
Physical examinations: A thorough examination of the head, neck, and nasal passages can help identify signs of sinusitis or nasal polyps.
Patient symptom histories: Detailed patient histories, including the frequency, duration, and characteristics of headaches, along with associated symptoms, can provide valuable information for diagnosis.
Treatment options for both conditions can vary widely and should be tailored to the specific diagnosis. Seeking care from a healthcare provider with experience in diagnosing and treating headaches is essential for accurate and effective management.
Conclusion
In summary, sinus headaches and migraines are two distinct types of headaches with overlapping symptoms that often lead to confusion. Understanding the differences between these conditions is crucial for receiving appropriate treatment and improving the quality of life for those affected. Accurate diagnosis by a healthcare professional is the first step in managing these conditions effectively.
The impact of misdiagnosis on a patient’s well-being and the potential for ineffective treatments underscore the importance of seeking professional guidance when faced with persistent headaches. If you or someone you know is experiencing recurrent headaches, consult a healthcare provider to determine the underlying cause and develop a personalized treatment plan.
In closing, we urge readers to prioritize their health and well-being by seeking medical attention when faced with chronic or severe headaches. Accurate symptom reporting and open communication with healthcare professionals are essential for an accurate diagnosis and the most effective treatment possible. Don’t let headaches stand in the way of a pain-free and fulfilling life; act now to seek the help you deserve!
Contact us for an appointment today!